This is the central access point for all Interactive Tools and Downloadable Resources from the AdvaNCe Health Together CCBHC certification program. It organizes additional learning materials from every Learning Track into a single, accessible hub, sorted into their respective tracks. Use the Navigation buttons above to jump to a specific section.
Interactive Tools
Track 1: Workflow Design to Optimize Clinical Talent
Track 2: Financial Management Of Prospective Payment & Value-Based Reimbursement
Track 3: Integrated Care Management & Care Coordination Excellence
Downloadable Resources
Track 1: Workflow Design to Optimize Clinical Talent
1.2.1-Task-Logger
The purpose of this log is to identify non-clinical tasks that consume provider time, quantify wasted capacity, and create a baseline for delegation and workflow redesign. By carefully logging and analyzing provider activities, teams can see where valuable clinical time is being lost and how to reassign tasks to maximize efficiency.

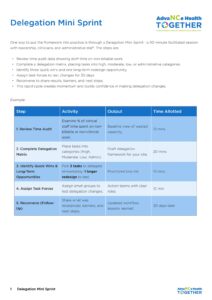
Downloadable Asset – 1.2.2 – Delegation Mini Sprint
The purpose of the task delegator is to help providers and managers categorize tasks based on complexity and necessary qualifications, ensuring safe reassignment while protecting clinical quality. Delegation allows clinicians to practice at the top of their license while empowering peers and support staff to contribute meaningfully.

1.2.4-Monitoring-and-Refinement-Tool
The purpose of this worksheet is to ensure that delegation and workflow improvements don’t stop at the design stage. Monitoring is about consistently measuring performance and making refinements when gaps or new challenges appear. Effective monitoring helps teams sustain progress, avoid backsliding, and continuously improve.
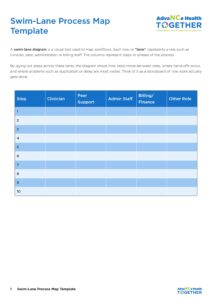

1.3.1 – Swim-Lane Template
A swim-lane diagram is a visual tool used to map workflows. Each lane represents a role such as clinician, peer, administrator, or billing staff. The columns represent steps or phases of the process. By laying out steps across these lanes, the diagram shows how tasks move between roles, where hand-offs occur, and where problems such as duplication or delay are most visible.

1.4.4 – Templates for Documentation
To reduce variability, organizations should provide fillable templates for peers and supervisors. Standardized templates also promote consistency across programs and sites, ensuring documentation is equitable, uniform, and audit-ready regardless of location or staff member.

1.4.5-Performance-Metrics-Feedback-Loops
The purpose of this module is to show how programs can measure the impact of peer roles and use structured feedback loops to continuously improve. Metrics tell us what is happening; feedback loops help us refine how we respond. Together, they ensure that peer integration is not a one-time initiative but an ongoing cycle of accountability and learning.

1.5.5-Improvement-Checklist
This improvement checklist will assist in the structured improvement cycle. Healthcare dashboards are powerful tools for visualizing key metrics, tracking performance, and supporting decision-making in clinical and administrative settings. But to ensure your dashboards remain relevant, accurate, and actionable, organizations should adopt a structured improvement cycle for continuous evaluation and enhancement. By embracing ongoing evaluation and refinement, healthcare organizations can maximize the utility and impact of their dashboards.
Track 2: Financial Management Of Prospective Payment & Value-Based Reimbursement
2.1.4-CCBHC-Comparative-Analysis-Matrix
Understanding how different reimbursement structures shape clinical, operational, and financial performance is critical for CCBHCs. A simple comparative matrix helps learners identify who carries financial responsibility (The payer, the CCBHC, or both) as well as what strategic advantages or challenges arise for a CCBHC when moving from volume-based payment (fee-for-service) to capitated or prospective payment models. This knowledge drives stronger decision-making, promotes financial sustainability, and ensures high-quality, person-centered care.

2.3.2 – Downloadable FAQ – Shared Expenses for CCBHCs
This FAQ outlines common shared (indirect) expenses for Certified Community Behavioral Health Clinics (CCBHCs). These categories align with SAMHSA, HRSA, and Medicaid PPS guidance and are essential for cost allocation, PPS rate development, and capitation modeling.

2.4.2-Forecasting-tool
The purpose of the model is solely to display information that can be gathered with minimal effort and can project outcomes. This function allows one to make small adjustments before larger ones are needed. Strong organizations will want to use models that are substantially more elaborate and detailed than the one provided to ensure the most accurate results

2.4.3-Quality-Metric-Reporting-format
The model is designed to show the standard reporting format for quality metrics. It is designed for ease of use and ease of understanding – both of which are key for quality departments using the data, It contains only two related variables. For clarity, others should be reported on other sheets. It also provides both numeric and graphic displays of results. visual graphic displays are generally better for understanding

2.5.2-2-x-2-scenario-planner
Both models in this file are ways to take the first step in scenario analysis, which is to define a series of scenarios that staff and others can react to and in calm and deliberate times make decisions that could be far more pressured in times of crisis. Both rely on a selection of variables. A variable is a driver or factor about the future that presently concerns you. The 2 X 2 matrices is a standard method that can be used quickly to create reasonably complex situations.

2.5.3-Sensitivity-Analysis
Traditionally sensitivity analysis is keyed on one or at the maximum two variables. The variable is flexed by providing possible numeric outcomes and testing each for the likely financial outcome for each item. Sensitivity analysis works best on objective numeric values as its goal is to define objective outcomes. In this example the reduction in Medicaid referrals that are due to changes in eligibility is reviewed.

2.5.4-Scenario-Analysis
This scenario analysis is based on combining two models. Likely these models were prepared by two different groups. The first group did the brainstorming of scenario planning and suggested a response of increasing productivity. As the work is different, the two groups likely did not meet in a single meeting. The second group added a new line for data entry. This line adds back increasing levels of productivity to replace the lost service volume. The two groups need to rely on the skills of each to assure that the amount of reductions and increases in service are both within possible ranges.

2.6.5 – Early-Warning Thresholds & Executive Escalation Protocols
Early-warning thresholds ensure that Medical Loss Ratio (MLR) and related financial/utilization metrics are monitored closely. Escalation protocols guarantee timely executive awareness and action before risks escalate. This tool reviews both.
Track 3: Integrated Care Management & Care Coordination Excellence
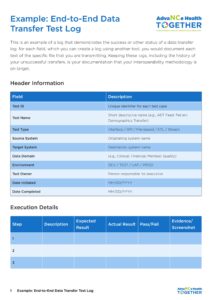
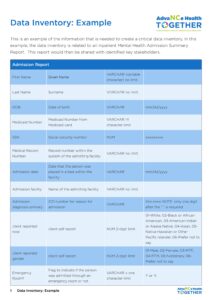
3.2.5 – Example – End to End Data Transfer Test Log
This is an example of a log that demonstrates the success or other status of a data transfer log. for each field, which you can create a log using another tool, you would document each test of the specific file that you are transmitting. Keeping these logs, including the history of your unsuccessful transfers, is your documentation that your interoperability methodology is on target.

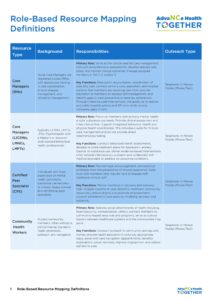
3.3.2 – Multidisciplinary Contributor Map
A multidisciplinary contributor map ensures that all team members involved in patient care understand their roles, responsibilities, and communication pathways. This guide provides a step-by-step approach for building and applying a contributor map in your organization.

3.3.3 – Integrated Care Plan Example For NC Tailored Plans
This example care plan template aligns with NC DHHS guidance and ISP requirements by integrating physical, behavioral, and social needs into one shared document. It lists member demographics, strengths, goals and interventions with assigned team members and timelines, meeting NC Targeted Case Management documentation standards for roles, outcomes, and progress tracking.

3.3.4 – NC Tailored Plan Assessment & Reassessment Protocol
This resource aligns with North Carolina Tailored Plan requirements for initial assessments and reassessments. It provides structured guidance to ensure timely, comprehensive care planning and documentation across behavioral health, physical health, and social determinants of health.

3.3.5 – NC Tailored Plan Behavioral Health Team Huddle & Case-Review Template
This template guides regular team huddles (case conferences) for NC Tailored Plan behavioral health care teams. Per NC Medicaid Tailored Care Management (TCM) requirements, care managers must hold regular interdisciplinary case conferences (aka team huddles/planning meetings) to coordinate member care, communicate across settings, and update the shared care plan.

3.4.4 – Transition Checklist
This checklist provides a guideline for sharing critical information at points where a member’s care is transferred between care settings or care professionals and service providers. It can be used as a standalone checklist or incorporated within an EHR or care management platform.

3.4.5-Performance-Monitoring-Audit-Asset
This tool demonstrates the metrics and components for developing Key Performance Measures for various standards in the CCBHC and TCM programs. It is intended to support organizations in monitoring their own performance and preparing for audits by regulatory entities.

3.5.2-Dynamic-Benchmark-configuration
The CCBHC Criteria Assessment is designed as a performance improvement resource to help engage CCBHCs in a self-reflective process specific to enhancing the criteria required for a Certified Community Behavioral Health Clinic (CCBHC). It is designed primarily as a performance improvement resource to increase an organization’s awareness of the CCBHC criteria and to engage in a self-reflective process that assists in identifying action steps moving forward.
Track 4: Technology, Data Architecture & Performance Management

4.1.5 – Handout Data Management Quality Assurance (QA)
The purpose of Data Management Quality Assurance (QA) is to ensure that data is accurate, complete, consistent, secure, and reliable throughout its lifecycle. QA practices reduce errors, enhance compliance, and support effective decision-making.

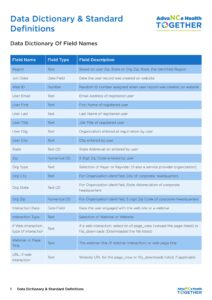
4.2.1 – Data Catalog Governance Coverage
A data catalog is a central inventory describing data assets across the organization. It ensures users can locate, understand, and trust the data they work with. In healthcare, a well-governed catalog links data to business meaning, stewardship roles, and compliance controls.

4.2.2-Data-Governance-Roles-and-Responsibilities-
Roles ensure data is defined consistently, validated accurately, and protected effectively. Effective data governance depends on clearly defined roles and responsibilities. Assigning ownership, stewardship, and technical administration ensures that data definitions, quality checks, and approvals are performed consistently and transparently across the organization.

4.2.4 – SDOH Screening Reporting in Behavioral Health
This summary template provides a standardized structure to complement a Social Determinants of Health (SDOH) report for behavioral health programs. The template focuses on the screening tool used, eligible population, completed screenings, and defined exclusion criteria.

4.2.5 – Quality Assurance (QA) & Issue Resolution Guide
Quality Assurance (QA) and issue resolution processes are critical to maintaining the accuracy, completeness, and reliability of governed data. QA ensures that data meets established standards, while issue resolution provides a structured method for identifying, documenting, and correcting problems.

4.3.1-CCBHC-Comparison-Matrix
The CCBHC Criteria Assessment is designed as a performance improvement resource to help engage CCBHCs in a self-reflective process specific to enhancing the criteria required for a Certified Community Behavioral Health Clinic (CCBHC). It is designed primarily as a performance improvement resource to increase an organization’s awareness of the CCBHC criteria and to engage in a self-reflective process that assists in identifying action steps moving forward.

4.4.4-How-To-Best-Deliver-KPI-Dashboards-For-Leadership
These are a list of main delivery options of KPI dashboards with strengths, limitations, and best uses. Effective delivery of KPI dashboards depends on choosing the right method to assure that leadership will use the information. Executives need access to timely, actionable, and clear information in formats that fit their workflow.

4.5.2-Bonus-eligibility-forecasting
This model is a sample of how to present rolling forecasts and use them to verify the plausibility of the work. Both the “Historical By Quarters” tab and the “Current Monthly Data” tab show data for a fictitious entity over time and uses that information to be more certain of their coming forecasts.

4.5.3-Quality-Bonus-Incentive-Data-Executive-Report
This model is a sample method for displaying monthly calculations of bonus incentive and providing them for review and adjustment by senior leadership. The sample page provides all the data needed for determination of next steps including the metric, the payment method, the benchmark needed for success, the prior historic rate that the company applied, and the actual YTD number.